Human cell atlas study reveals how the maternal immune system is modified early in pregnancy
The first Human Cell Atlas study of early pregnancy in humans has shown how the function of the maternal immune system is affected by cells from the developing placenta. Researchers from the Wellcome Sanger Institute, Newcastle University and University of Cambridge used genomics and bioinformatics approaches to map over 70,000 single cells at the junction of the uterus and placenta. This revealed how the cells talk to each other to modify the immune response and enable the pregnancy.
Published in Nature, this work presents new and unexpected cell states in the uterus and placenta, and shows which genes are switched on in each cell. Insights from this will help us to understand what leads to a successful pregnancy, and what can go wrong during miscarriages or pre-eclampsia.
Maintaining a healthy pregnancy can be difficult sometimes, with many women suffering from miscarriages or still birth, and others having problems such as pre-eclampsia. The roots of many of these problems occur in the first few weeks of the pregnancy, when the placenta is formed.
To understand this area, researchers studied more than 70,000 single cells from first trimester pregnancies. Using single-cell RNA and DNA sequencing they identified maternal and fetal cells in the decidua and placenta, and found how these cells were interacting with one another. They discovered that the fetal and maternal cells were using signals to talk to each other, and this conversation enabled the maternal immune system to support fetal growth.
“For the first time ever, we have been able to see which genes are active in each cell in the decidua and the placenta, and have discovered which of these could modify the maternal immune system. The fetal cells from the placenta communicate with the mother’s immune cells to ensure the placenta implants correctly. This allows the fetus to grow and develop normally.”
Dr Roser Vento-Tormo A first author on the paper from the Wellcome Sanger Institute
Using microscopy-based methods the researchers were also able to pinpoint the location of new cell states in the different layers of the decidua. They saw how the biological blocks of the placenta – called trophoblast cells – invade into the lining of the mother’s uterus and cause the tissue to change structure, creating the blood supply for the developing fetus.
“This study was only possible due to the Human Developmental Biology Resource, which provides tissues to enable research into understanding human development to help improve health. Our single cell study has shown us the exact cellular composition of the decidua and placenta for the first time, and how the cells from the developing placenta and uterus communicate. This has huge implications for understanding what happens in a normal pregnancy, and for studying what can go wrong during conditions such as pre-eclampsia and miscarriage.”
Professor Muzlifah Haniffa A corresponding author from Newcastle University
“The formation of the decidua is vital for a successful pregnancy and our study has revealed completely new subtypes of cells within the decidua. Further clarification of what each of these cells do will help to understand how the maternal immune response helps achieve a successful pregnancy.”
Professor Ashley Moffett A corresponding author from Cambridge University
Understanding this area also has implications for the study of cancers. Tumour cells can use similar mechanisms to evade the immune system and extract new blood supply to provide nutrients and oxygen for tumour growth.
“This first Human Cell Atlas of early pregnancy gives us a reference map of this vital initial phase of development. It will transform our understanding of healthy development, and is helping us understand how the placental and maternal cells communicate with each other to support pregnancy. This will shed light on disorders of pregnancy, and could also help understand pathways that cancer cells exploit.”
Dr Sarah Teichmann A corresponding author on the paper from the Wellcome Sanger Institute and co-chair of the Human Cell Atlas initiative Organising Committee
More information
Background information:
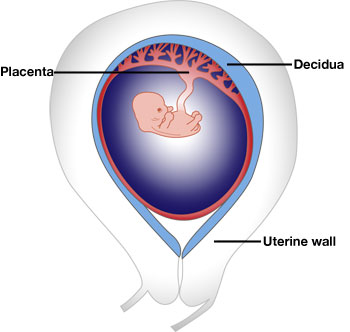
In pregnancy, the embryo is surrounded by a placenta that transports oxygen and nutrients from the mother. The placenta attaches to the lining of the uterus, known as the decidua. Placental cells – trophoblast cells – are fetal in origin and have its genetic make-up, which is different from the mother’s (maternal) cells. Trophoblast implant into the lining of the uterus to create the decidua, and invade to reach the specialised blood vessels in the wall of the uterus. This creates a vital blood supply for the placenta and the fetus.
The placenta acts as a no-man’s land between the mother and the fetus, and an immune compromise occurs here between these two genetically different individuals. This compromise allows for normal fetal growth and development.
Publication:
Roser Vento-Tormo & Mirjana Efremova et al. (2018) Single-cell reconstruction of the human early maternal-fetal interface Nature. DOI: 10.1038/s41586-018-0698-6
Funding:
This study was supported by Wellcome, the MRC, EMBO, the ERC, Human Frontiers and other funders. Please see the paper for the full list of funders.
Selected websites
About the University of Cambridge
The mission of the University of Cambridge is to contribute to society through the pursuit of education, learning and research at the highest international levels of excellence. To date, 98 affiliates of the University have won the Nobel Prize. Founded in 1209, the University comprises 31 autonomous Colleges, which admit undergraduates and provide small-group tuition, and 150 departments, faculties and institutions. Cambridge is a global university. Its 19,000 student body includes 3,700 international students from 120 countries. Cambridge researchers collaborate with colleagues worldwide, and the University has established larger-scale partnerships in Asia, Africa and America. The University sits at the heart of the ‘Cambridge cluster’, which employs 60,000 people and has in excess of £12 billion in turnover generated annually by the 4,700 knowledge-intensive firms in and around the city. The city publishes 341 patents per 100,000 residents. www.cam.ac.uk
Wellcome Sanger Institute
The Wellcome Sanger Institute is one of the world’s leading genome centres. Through its ability to conduct research at scale, it is able to engage in bold and long-term exploratory projects that are designed to influence and empower medical science globally. Institute research findings, generated through its own research programmes and through its leading role in international consortia, are being used to develop new diagnostics and treatments for human disease. To celebrate its 25th year in 2018, the Institute is sequencing 25 new genomes of species in the UK. Find out more at www.sanger.ac.uk or follow @sangerinstitute on Facebook, Twitter and LinkedIn
Wellcome
Wellcome exists to improve health for everyone by helping great ideas to thrive. We’re a global charitable foundation, both politically and financially independent. We support scientists and researchers, take on big problems, fuel imaginations and spark debate. wellcome.org