Sepsis patients could get the right treatment faster, based on their genes
Listen to this article:
Listen to “Sepsis patients could get the right treatment faster based on their genes 18 June 2024” on Spreaker.
Sepsis patients could be treated based on their immune system’s response to infection, not their symptoms.
New research uncovers how different people respond to sepsis based on their genetic makeup, which could help identify who would benefit from certain treatments and lead to the development of targeted therapies.
The team, from the Wellcome Sanger Institute, the University of Oxford, and collaborators, built on their previous work that identified different subgroups of patients with sepsis. They aimed to understand more about why sepsis response varies between patients and the different underlying immune response pathways.
The new study, published today (18 June) in Cell Genomics, details the genetic basis of variability in sepsis response, and the different regulators and cell types involved in the different immune responses in each subgroup of patients.
Having a more detailed understanding of sepsis at a molecular level could identify those who would benefit from different therapies, helping to design rapid tests, organise clinical trials, and develop targeted treatments based on the individual immune response.
The ultimate aim is for patients to receive the most effective treatment for their sepsis more quickly, based on their immune response rather than their symptoms. In the future, this approach to personalised medicine could also be applied to other less severe infections, not just sepsis.
Sepsis causes an estimated 11 million deaths worldwide per year, with one death every three seconds. In the UK alone, at least 245,000 people are affected by sepsis, and 48,000 people die each year.1
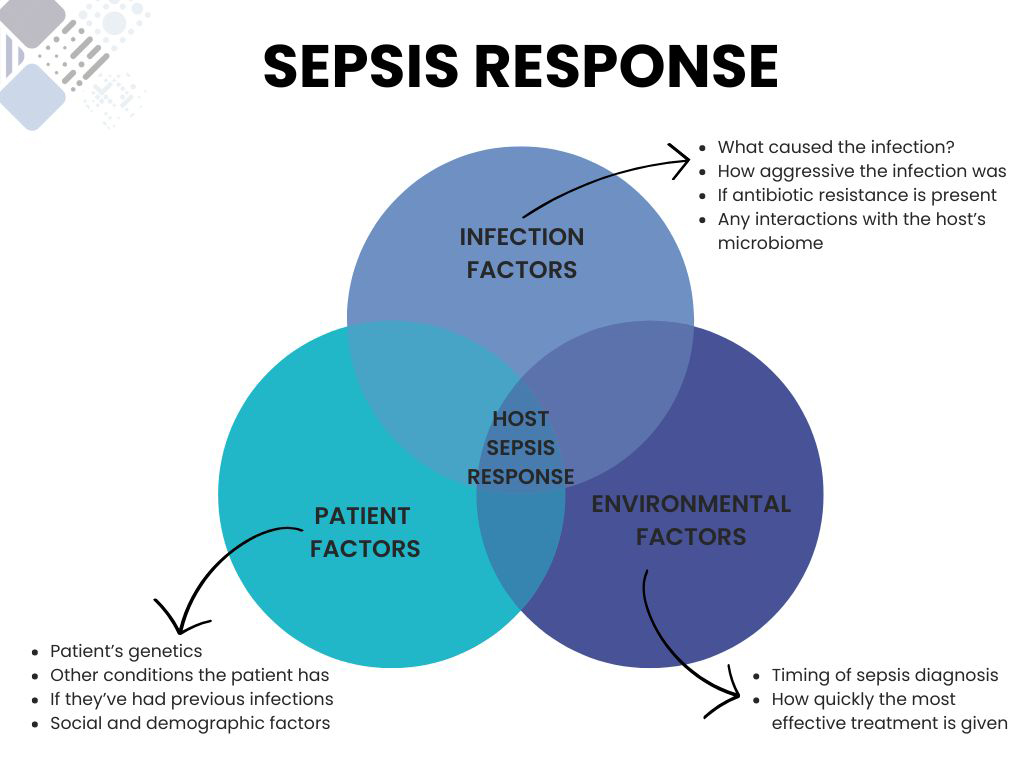
Sepsis arises when the body has an extreme response to an infection and injures its own tissues and organs. Sepsis can cause different downstream immune responses in different people. Depending on this immune response, the treatment varies. However, it is difficult to identify which response is happening based on symptoms alone. Sepsis can progress quickly, and if the wrong treatment is given, valuable time could be lost.
Previously, researchers from the Wellcome Sanger Institute, the University of Oxford and collaborators, identified how expression of a small set of genes allowed them to categorise who was most at risk from poorer outcomes from sepsis and COVID-192.
Building on their previous work, in this new study the team investigated the impact of genetic variants that regulate gene expression, known as expression quantitative trait locus, or eQTLs. This provides insight into how an individual’s genetic makeup could influence the way they respond to sepsis. This information can help classify who would benefit from targeted therapies, which act on the immune system in different ways.
The team analysed data from the UK Genomic Advances in Sepsis (GAinS) study that contained 1,400 patients with sepsis due to community-acquired pneumonia and faecal peritonitis3 from intensive care units across the UK.
They found that genetic variation in groups of patients is associated with differences in immune response during sepsis. They then used this to identify key genetic regulators in each group, helping to describe what biological networks, cells, and mechanisms are involved in each response.
Understanding the regulatory networks underlying the different patient responses provides additional information for developing treatments that work with the immune system and are a step towards a personalised medicine approach to treating sepsis.
In related research, rapid tests that identify different subtypes of sepsis are also being developed by Dr Julian Knight at the University of Oxford4. These aim to quickly show those who would benefit from targeted treatments.
The next steps would be to further investigate the immune response to find targeted treatments for each immune response or different stages of the immune response.
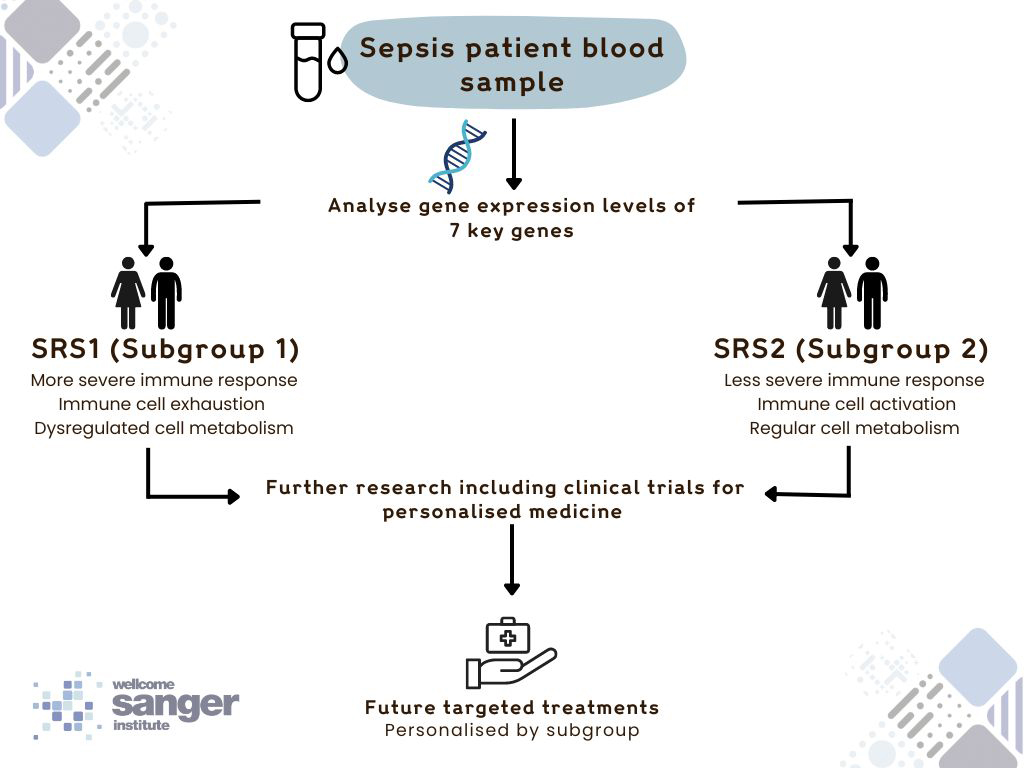
“Our study is the next step towards being able to treat sepsis based on someone’s genetics and their particular immune response, instead of their symptoms, which can vary greatly from person to person. Our research found two groups of people, with opposite immune responses, and identified the genetic regulators involved. Being able to molecularly categorise patients with sepsis allows clinicians to correctly identify who could benefit from the available treatments and gives new direction to those developing targeted therapies.”
Dr Katie Burnham, first author from the Wellcome Sanger Institute
“Understanding who is at greater risk from sepsis and how they respond to the disease is a huge task. Research such as this, that dives deeper into the molecular basis of the disease, aids in the ongoing development of tests that could identify different subtypes of sepsis and allow medical professionals to treat this straight away. Our research can be directly translated into the clinic and we hope that it allows us to start to develop an efficient, targeted approach to treating this life-threatening disease.”
Dr Julian Knight, co-senior author from the University of Oxford
“Sepsis is a complicated and devastating disease that impacts millions of people around the world each year. Understanding the molecular processes that happen during sepsis, and how genetics plays a role in this, can help give answers to long-standing questions, improve patient outcomes, and allow for the development of effective clinical trials that lead to new targeted treatments as quickly as possible.”
Dr Emma Davenport, co-senior author from the Wellcome Sanger Institute
More information
- The UK Sepsis Trust. Available at https://sepsistrust.org/about/
- https://www.sanger.ac.uk/news_item/sepsis-and-covid-19-patients-most-at-risk-predicted-with-genetic-model/
- Community-acquired pneumonia is when someone catches pneumonia outside of a healthcare setting, while in the community. Faecal peritonitis is when the thin layer of tissue inside the abdomen becomes infected by faecal matter.
- This work is in partnership with the Danaher Corporation. More information can be found here: https://oxfordbrc.nihr.ac.uk/partnership-with-danaher-paves-way-for-precision-medicine-test-for-sepsis/
Publication:
K. Burnham, N. Milind, W. Lee, et al. (2024). eQTLs identify regulatory networks and drivers of variation in the individual response to sepsis. Cell Genomics. DOI:10.1016/j.xgen.2024.100587
Funding:
This research was funded by Wellcome, the Medical Research Council, and the Winston Churchill Foundation. A full acknowledgement list can be found in the publication.